This blog explains the updated understanding of diabetes insipidus, why its name is changing, and how a new test using copeptin can improve diagnosis. Aimed at students and professionals, it offers a clear summary of hormone regulation, diagnostic challenges, and how science is shaping safer, more accurate patient care.
By Ayyaz Ahmad – Deputy Training Lead & Specialist Biomedical Scientist
Published on LabPathPro.com
Many people have heard of diabetes, but fewer know about a condition called diabetes insipidus. Despite the similar name, it has nothing to do with blood sugar. Instead, it’s a rare condition that affects how the body manages water.
In a recent CPD seminar by the IBMS Birmingham Branch, a detailed talk explained how we diagnose this condition, why the name is changing, and how a new blood test called copeptin may make diagnosis easier and safer in the future.
This post is a simplified summary of that session — perfect for students, lab professionals, and anyone curious about how science helps diagnose complex conditions.
Why Is the Name Changing?
The name diabetes insipidus has caused confusion for decades. Many healthcare staff mix it up with diabetes mellitus, the common type linked to high blood sugar. But the two are very different:
- Diabetes mellitus: You pass sugary urine due to high glucose.
- Diabetes insipidus: You pass large amounts of very diluted (not sweet) urine because your body can’t keep water properly.
This confusion has led to serious mistakes in hospitals, including cases where patients didn’t get the right treatment in time. To help prevent harm, doctors now recommend changing the name to:
- AVP Deficiency (central/cranial causes – the brain doesn’t make enough hormone)
- AVP Resistance (nephrogenic causes – the kidneys don’t respond to the hormone)
How Does the Body Control Water?
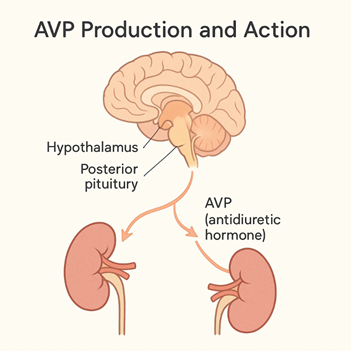
The brain produces a hormone called arginine vasopressin (AVP), also known as antidiuretic hormone (ADH). It helps the body keep the right amount of water by:
- Telling the kidneys to hold on to water (especially when we’re dehydrated)
- Narrowing blood vessels during low blood pressure to maintain circulation
This balance keeps your blood sodium level and osmolality (water-salt balance) within a healthy range.
What Happens in Diabetes Insipidus?
In people with diabetes insipidus (now called AVP Deficiency or Resistance):
- They pass huge amounts of clear urine (over 4–5 litres a day)
- They feel extremely thirsty, sometimes needing to drink constantly
- Their urine is dilute, and their blood sodium may rise dangerously
There are three main causes:
- AVP Deficiency (Central DI) – The brain doesn’t produce enough hormone
- AVP Resistance (Nephrogenic DI) – Kidneys ignore the hormone
- Primary Polydipsia – The person drinks too much water, usually linked to mental health conditions
How Do We Currently Diagnose It?
The Water Deprivation Test is still the most used method. It involves:
- Stopping all fluids for several hours
- Taking regular samples of blood and urine
- Measuring how well the body concentrates urine without water
If the body fails to concentrate urine despite high blood salt levels, this suggests diabetes insipidus. A dose of desmopressin (synthetic AVP) is then given to see if things improve — this helps tell whether the problem is in the brain or kidneys.
But the test is:
- Long and uncomfortable for patients
- Difficult for laboratories to coordinate
- Only about 70% accurate
What Is Copeptin and Why Does It Matter?
Copeptin is a small protein released in equal amounts with AVP. But unlike AVP, copeptin is much more stable and easier to measure in the lab.
That makes copeptin a very helpful indirect marker of AVP levels.
Researchers have found that:
- Very high copeptin levels (above 21.4 pmol/L) = AVP Resistance (nephrogenic DI)
- Very low levels (below 4.9 pmol/L) = AVP Deficiency (central DI)
- Normal or high levels after salt infusion = Primary Polydipsia
How Does the New Test Work?
To make the test more accurate, doctors give a hypertonic saline infusion (a strong salty drip) to raise the blood sodium above 147 mmol/L.
Then, they measure copeptin:
- If it’s low, the brain isn’t making AVP → AVP Deficiency (treat with desmopressin)
- If it’s high, the kidneys are ignoring AVP → AVP Resistance
- If it’s normal or high, the problem is too much water drinking → Primary Polydipsia
This method gives up to 96% accuracy — much better than the water deprivation test.

Real Case Example
An 18-year-old girl had extreme thirst and passed 4 litres of urine daily. Her initial water deprivation test results were unclear. Her blood sodium didn’t go high enough, and urine was only partly concentrated.
To avoid misdiagnosis, she had the copeptin test after a salt infusion. Her level was high, showing that her brain was making enough AVP — it was Primary Polydipsia, not diabetes insipidus. She was referred for mental health support instead of being wrongly started on lifelong medication.
Final Thoughts
The copeptin test could transform how we diagnose diabetes insipidus. It’s more accurate, safer for patients, and easier to interpret. Although it’s not yet used in every hospital due to cost and logistics, it has great potential.
As Biomedical Scientists, we must stay informed about these advances — not only for our practice but to advocate for better care.
Further Reading & References
- Fenske W, et al. Annals of Clinical Biochemistry, 2024
- UK Endocrine Society Guidelines
- NHS Patient Safety Alert (2016)
Sign up for free class
It’s easy and free!










